

Dry skin
Effective moisturisation for dry skin

Very dry skin
Clinically proven to treat and soothe dry skin conditions
Specialised treatments
Specialised treatments for skin conditions

Facial Skin
Daily care for dry and sensitive faces
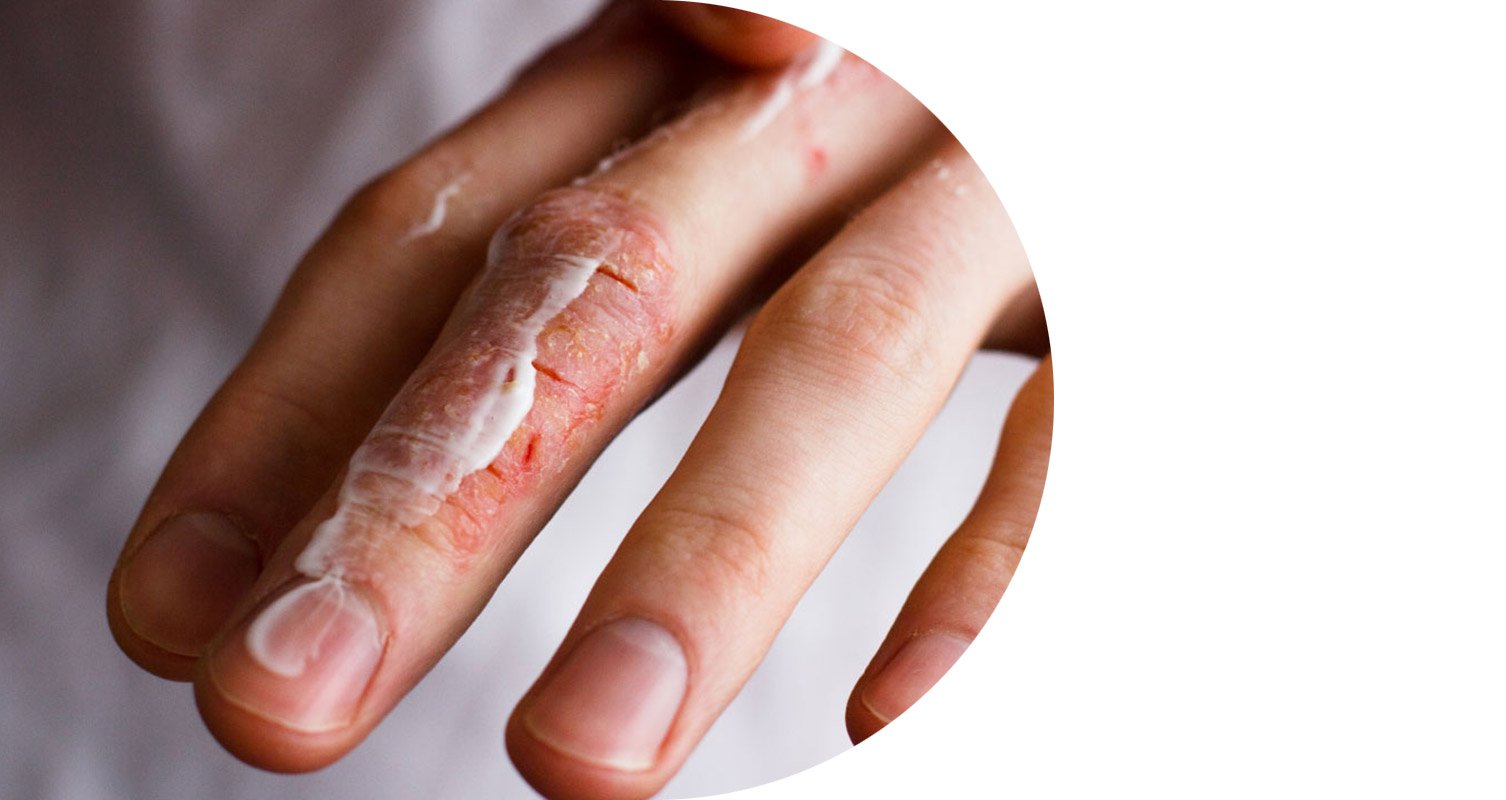
Eczema
Eczema is a condition where patches of skin become dry, itchy, inflamed, cracked or sore. It can appear on any part of the body, but most commonly affects the hands, elbows, knees, face or scalp.
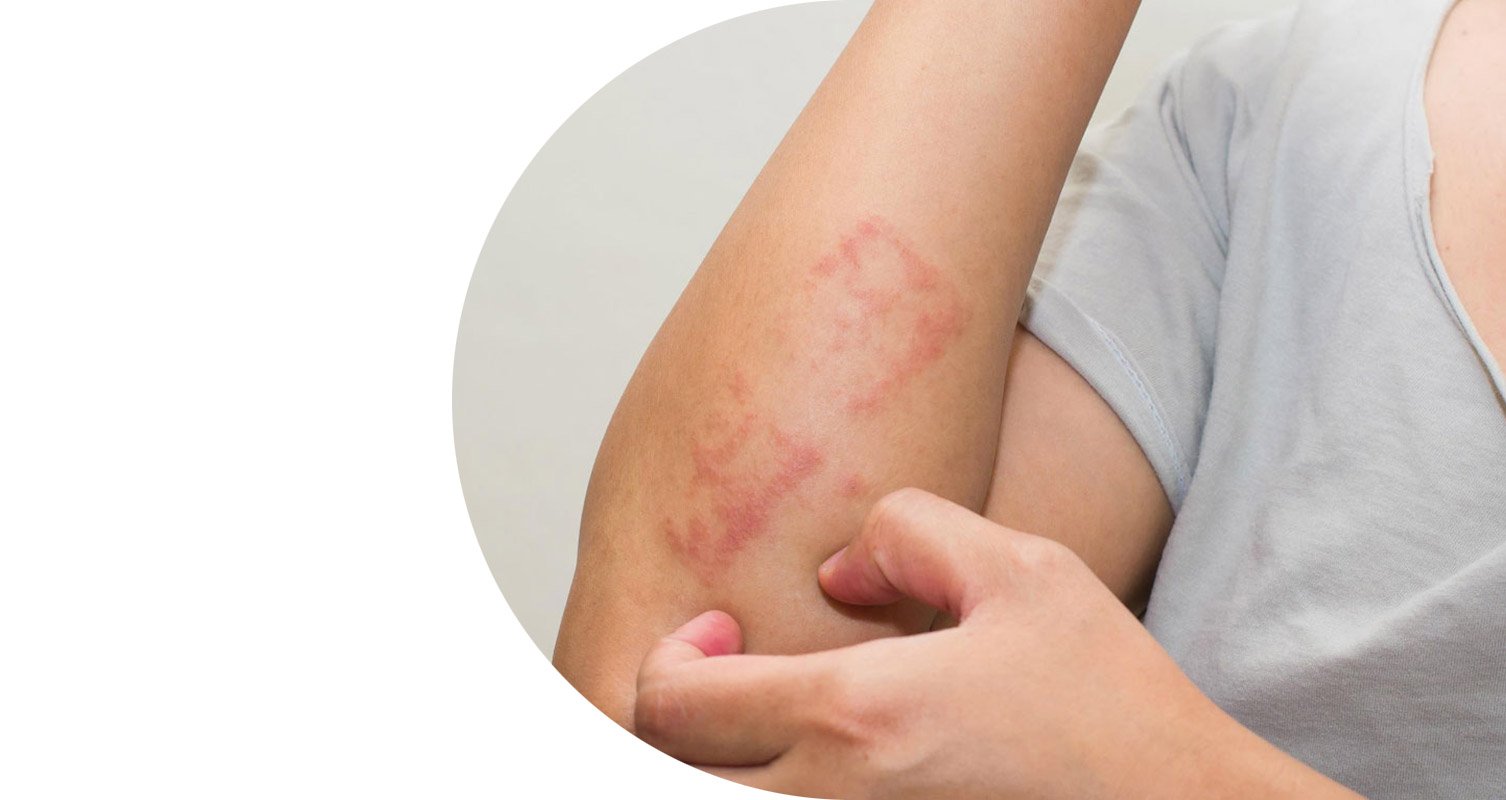
Itchy skin
Itchy skin is a common irritating sensation that makes you want to scratch. This can happen anywhere on your body. Sometimes, the itch is caused by dry, cracked or irritated skin.

What is an emollient?
Emollients are effective moisturising treatments for protecting and rehydrating skin that’s dry, itchy or scaly. They can help you manage symptoms of skin conditions such as eczema, dermatitis, psoriasis and ichthyosis.










































